As the healthcare ecosystem has evolved over the years, one of the major feats has been the acceptance and evolution of patient monitoring systems to augment patient care and improve clinical performance. Assessing the condition or other medical parameters of a patient is essential in making informed clinical decisions.
Parameters such as patient identity protection also plays an important role to prevent the identity theft of patients. Through the medicare beneficiary identifier (an 11-character patient identification number), the identity of patients in Medicare transactions can be improved and protected.
Patient monitoring inside and outside the hospital plays an important role in this process, as the infrastructure connects different modules of the healthcare ecosystem for effective patient care.
This article addresses the advantages of remote patient monitoring, the shift toward wearables and other wireless-based systems for patient monitoring with examples of current systems, and the factors driving innovation and investment in the healthcare segment.
“Monitoring” in medical terms attributes to observation of a condition, disease or several medical parameters over time. Assessing the patient’s condition, or any other medical parameters, to make informed clinical decisions supports the need for better patient monitoring. The healthcare ecosystem has evolved over years. One major feat has been the acceptance and evolution of patient monitoring systems to augment patient care and improve clinical performance. Physiological signals hold information that can be extracted to identify the functioning state of various bodily systems.
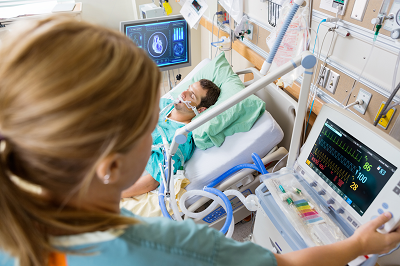
Throughout treatment, it is extremely important to monitor the vital physiological signs of a patient on a continuous basis. Consequently, patient monitoring systems have always occupied a very significant position in the arena of medical devices. The increasing medical needs and growing demand for medical facilities are likely to drive patient monitoring systems future market growth.
Monitoring Classifications
Patient monitoring systems can be classified in several ways. Common types are measured parameters and medical use cases. The classification based on measured parameters categorizes the monitoring systems into two broad categories – single parameter monitoring and multi-parameter monitoring. Single parameter systems can measure only single physiological signals like blood pressure, ECG, SPO2, and CO2. Multi-parameter monitoring systems can measure a combination of vital signals like ECG, respiration rate, blood pressure, SPO2, brain waves, gas anesthetic concentration, and body temperature.
Alternatively, the classification based on medical use cases categorizes the patient monitors as follows:
- Blood glucose monitoring
- Hemodynamic monitoring – continuous cardiac output (CCO), stroke volume (SV), stroke volume variation (SVV), pulse pressure variation (PPV), mean arterial pressure (MAP), and systemic vascular resistance (SVR)
- Neurological monitoring – brain Waves (EEG and EMG), gas anesthetic concentration, bispectral index
- Cardiac monitoring – ECG
- Body temperature monitoring – thermometry
- Respiratory monitoring – pulse oximetry & capnography (CO2)
- Fetal and maternal monitoring – maternal and fetal heart rate
Infrastructure
A typical patient monitoring system consists of one or more sensors, processing components, display devices and communication links for displaying or recording the results elsewhere through a monitoring network. Sensors used in the setup can be optical, electrochemical, electrodermal, or pressure and strain gauge. The processing and display components comprise microcontroller units (MCU) that can handle analog signal conditioning, digital signal processing, motor control, LCD control, touch sensing, wired and wireless connectivity.

On the communication front, several patient monitoring units are networkable, i.e., they can send their output to a central nursing station where an individual staff member can monitor and respond to multiple bedside monitors simultaneously. Different healthcare standards have been developed by organizations like IEEE and HL7 to facilitate integration of physiological data from patient-monitoring networks into hospital electronics’ health record and digital charting systems.
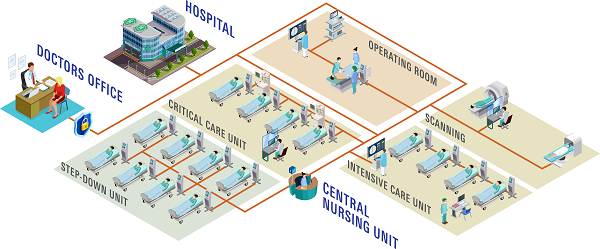
Patient Monitoring System Infrastructure
Wired to Wireless
Healthcare providers are continuously seeking innovative products to enhance patient care for a growing population. As they explore these solutions, a key question arises: what is RPM software? Remote Patient Monitoring (RPM) software utilizes digital devices and wireless technology to enable healthcare professionals to monitor patients’ health status remotely. This approach facilitates paramedics, clinicians, and medical personnel with hands-free devices to monitor a patient’s vital signs, creating a safer environment for both EMS personnel and patients.
Patient data can be transferred through a remote system from the ambulance to hospital to give doctors, nurses and other staff better situational knowledge prior to a patient’s arrival. A major advantage of Wi-Fi based monitoring is that it allows hospitals to leverage existing IEEE 802.11 (Wi-Fi) wireless network infrastructure and investment. Sixteen percent of U.S. Hospital and Health Systems have already implemented Wi-Fi based wireless patient monitoring and the coverage is expected to jump to 34 percent in the next few years. A major driving factor is the FDA 510K approval for recently introduced wireless monitoring devices. Low-acuity wearable patient monitoring devices with wireless capability are gaining recognition. They are compact, rechargeable and provide secure wireless connectivity.
Similarly, implantable cardiac monitors that are used for long term monitoring of a patient’s heart electrical activity have secured FDA approval. These implantable monitors can be connected to smartphone via Bluetooth. The technology provides a new way to monitor for atypical heart rhythms, while staying connected to the doctor remotely.
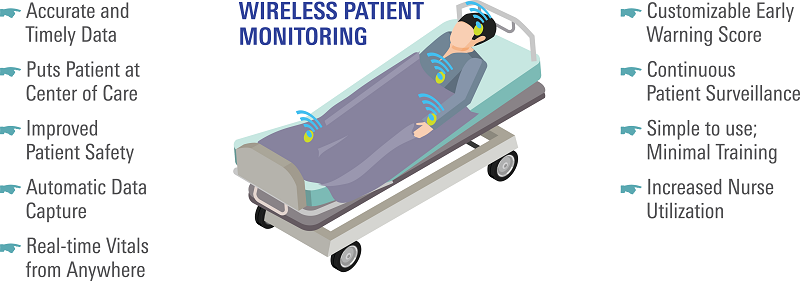
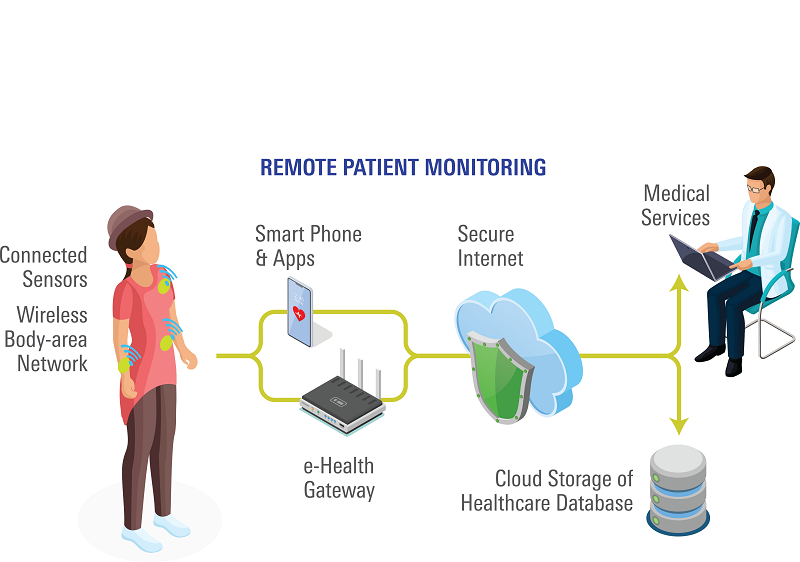
Remote Patient Monitoring (RPM)
RPM uses digital technologies to collect medical and other forms of health data from individuals in one location and electronically transmit that information securely to health care providers in a different location for assessment and recommendations. One example of such technology is a healthcare virtual assistant, which is capable of managing several areas of data collection and communication all at once. The RPM concept aligns well with the point of care shifting from a hospital to a patient’s home. A typical remote patient monitoring system will include a health hub used as the gateway device to collect and transmit vital sign measurements to the healthcare provider.
The market for RPM solutions remain in a state of development. While growth is appreciable, the overall adoption is still low in comparison to the total number of chronic patients. The acceptance of RPM has been mainly in North American and Western European regions where the healthcare providers are incentivized to keep the readmission rates low.
Future Trends
A patient monitor is considered the “data powerhouse”, capable of accumulating a significant amount of patient data. As the healthcare industry changes to improve competence in providing high quality patient care, there is growing demand for data integration and analytics to improve patient diagnosis and workflow. The future rests in understanding how patient data can fuel new product innovations, and be utilized in artificial intelligence algorithms within healthcare. Rather than making decisions on cloud-based data, emergency protocols could be implemented through decisions made on edge-node data. Moving forward, edge node computing combined with wireless patient monitoring will be considered an advantage for life critical applications.
About the Author

Dev Mandya is a Senior Segment Marketing Manager at Renesas Electronics America Inc. Dev holds a Master of Science degree in Electrical Engineering from the University of Southern California, Los Angeles.